(Continued from Part 1. This concludes the article.)
Stockpile Medical Supplies:
- Basic Household First Aid Kits: These are essential for treating the very minor/nuisance injuries one encounters in their daily lives. This is not as comprehensive as any prepper should have on hand, but its low cost is a starter towards having some medical supplies on hand. Many of the items could prevent worse problems, such as Neosporin preventing a life-threatening infection in a TEOTWAWKI situation. (These kits can be obtained at virtually any retailer for under $20.)
- More Comprehensive First Aid Kits: Useful for someone with slightly more advanced medical training than the non-medical lay person. These can be purchased online (from prepper or EMS websites, Amazon, or by assembling your own kit from a “shopping list”)
- IFAK (“Individual First Aid Kit”):
- Commonly used in military and tactical EMS applications. They are usually packaged in a MOLLE style pouch that can attach to a tactical bag.
- There are many variances, but all are designed to be used in an austere environment and provide life-saving, but often times not definitive, care.
- At a minimum, these kits need: tourniquets (at least 2), CPR mask, gloves, Kwik-Clot gauze, and chest decompression needles (at least 2).
- Every prepper (each member of the family/group) should own his/her own kit, keep it stocked, and know how to use it. My wife and I keep a kit in each vehicle, since we believe that most preparedness skills will be far more likely needed at an “everyday” emergency, than the possibility there will be a total breakdown of our medical system with care unavailable in a WTSHTF. Each member who carries their kit in a vehicle should also maintain a duplicate IFAK for their plate carrier/bug out bag (BOB) or remember to get the IFAK attached to their BOB if TEOTWAWKI occurs.
- Advanced/Specialized Medical Supplies:
- This can range from sutures for wound management, surgical instruments, diagnostic tests, casting/splinting supplies, to antibiotics, etc.
- Most of these purchases should depend on the level of training of someone in the preparedness group, or someone who you reasonably anticipate at your bugout location. (For instance, if your brother-in-law was likeminded and also happens to be a board-certified Emergency Physician, but lived 3 states away, you might want to stock up on more pre-positioned advanced medical supplies, if your in-laws’ plan was to bug out to your retreat in a TEOTWAWKI situation. He might even have access to antibiotics and other live-saving medication to add to the larder.)
- While I cannot legally advocate for anyone to practice medicine above his/her current scope of certification/licensure, I can also say that in a true WTSHTF situation there will be no licensing boards to restrain your actions. At that time, it may be an “every man for himself” world, and your family or friends’ lives may depend on your actions. So, by all means, read/attend seminars/watch YouTube videos on skills that may be useful in such a world. Just remember that you can do harm to a loved one if you do not know what you’re doing, so I would encourage you to learn, train, and continually practice.
- I highly suggest learning about wound management (including disinfection/ irrigation and debridement/ suturing) and having an abundance of supplies on hand to attend to such wounds. These will be frequently seen in a TEOTWAWKI scenario.
- CPR Equipment and an AED:
- CPR equipment (Ambu bag/mask, oral or nasal airway, or pocket CPR shield) is useful so that the rescuer is not exposed to body fluids on the patient they are rescuing.
- AED (automated external defibrillator): AED’s are now found in many public places and can also be purchased for private residences or small businesses. This is a worthwhile skill to have in the event that anyone around you experiences a cardiac arrest.
- An AED is not a cheap investment (they cost close to $1,000) but early defibrillation saves many more lives than just doing chest compressions, so the question might be, how much would you pay to have an AED in your hand if your loved one just collapsed with a cardiac arrest, and you have 4-6 minutes to save their life?
- The more remote you live from EMS services and/or the more that members of your family or preparedness group have a history of cardiac issues/risk factors, the more I would recommend emphasizing an AED purchase as part of your preps.
Train Up, Practice Up:
- Basic medical preparedness should be a mission of everyone in the group. No matter whether you are in a medical profession or not, there is a high statistical probability that you will encounter a medical emergency situation at some point in your life. It is also likely that this emergency will involve a family member, friend, or co-worker.
- There are many free or low-cost training opportunities available, and these are offered throughout the U.S. on a regular basis. The time commitment is often minimal, usually 1-2 nights total for CPR or Stop the Bleed.
- I strongly encourage everyone, whether in a medical profession or not, to at a minimum become trained in two things: CPR and Stop the Bleed.
- CPR:
- Make sure this course also has instruction on the use of AED’s.
- This course is offered by both the American Heart Association and the Red Cross.
- CPR:
- Stop the Bleed (aka- “Bleeding Control” or “B-CON”):
- This course covers tourniquet application, packing of wounds, and other techniques useful in everyday life as well as prepping. It would be useful in the event of gunshot or knife wounds, chainsaw accidents, or motor vehicle accidents.
- Again, the more rural you live, the more useful this skill becomes in everyday life as you may be the first person that happens upon such an injury long before EMS arrives, and stopping the bleeding can save a life.
- The curriculum was developed by the American College of Surgeons in response to recent mass casualty/active shooter incidents where trained bystanders would have been able to save lives from early bleeding control.
- https://www.bleedingcontrol.org
- This course covers tourniquet application, packing of wounds, and other techniques useful in everyday life as well as prepping. It would be useful in the event of gunshot or knife wounds, chainsaw accidents, or motor vehicle accidents.
- First Aid Course: Red Cross offers a First Aid course for the layperson. It would be a good basic course for everyone in your group to attend as well if they are not in the medical profession. (https://www.redcross.org/take-a-class)
- Emergency Medical courses:
- There are multiple courses available to those who wish to further their medical knowledge in the EMS arena. They are, in increasing order of training/hours required: (https://www.nremt.org/rwd/public/)
- EMR (Emergency Medical Responder): The equivalent of a “First Responder” course. Many volunteer firefighters and police officers are certified in this as they are tasked with rendering basic life-saving maneuvers until more definitive EMS help can arrive.
- EMT-B (Emergency Medical Technician-Basic; aka- “EMT”): This course usually can be completed in a few months by going a few hours/week. It is a mix of classroom and hands-on skill stations, and also requires observation shifts with both a Fire/EMS service and in an Emergency Department at a hospital. It would be a useful skill for at least 1-2 members of your group to have.
- EMT-A (Emergency Medical Technician-Advanced): This course provides additional training (especially hands-on) to the EMT-B skills set. It allows EMT-A’s to render a broader range of therapies under many EMS systems’ protocols. (https://survivalblog.com/advanced-emt-preppers-r-s/)
- EMT-P (Emergency Medical Technician-Paramedic; aka- “Paramedic” or “Medic”): This is a large time commitment and often only undertaken by those in the EMS/Fire/Hospital professions. It will provide a graduate with a large fund of knowledge and skills, and also has rigorous CME (continual medical education) requirements. The time commitment for training and maintaining a license would be difficult without at least part time work in one of these fields. Paramedics are excellent additions to a preparedness group, if they are otherwise a good philosophical fit with the group.
- Some state-level Emergency Medicine Agencies are providing low or no-cost EMR and EMT-B training to increase the number of laypersons with medical knowledge. This helps ease the cost burden for those who can take advantage of this opportunity and may also lead to work opportunities in the Fire/EMS field.
- Fire I and II courses are also publicly available for those who wish to have knowledge of how to deal with fire and rescue threats. These certifications are often membership requirements of (but often paid for by) volunteer fire departments, and also hiring criteria prior to interviews at many paid firefighting positions.
- There are multiple courses available to those who wish to further their medical knowledge in the EMS arena. They are, in increasing order of training/hours required: (https://www.nremt.org/rwd/public/)
- Dental, Nursing, CST, Pharmacy, and Allied Health Professionals:
- There are many licensed allied health professionals that can bring medical skills to your preparedness group.
- Dentists are the experts on tooth and gum disease, which will become much more prevalent in a TEOTWAWKI scenario. They also have advanced knowledge of dental matters, with some training in medical knowledge outside the mouth as well. Most dentists perform surgical skills (the breadth of these depends on their area of practice) which could be used elsewhere in the body in an emergency, and they often have access to antibiotics.
- Pharmacists will have knowledge of many of the medications (and possible substitutes) your group may have questions about. They may have some working knowledge of other medical topics if they have worked in a clinical setting.
- Nurses may bring a large fund of knowledge and skills with them to the preparedness group, largely depending on their work background. Experience in Surgery, Emergency Medicine, OB, or ICU would be ideal backgrounds for preparedness group members.
- CST’s (Certified Surgical Technologists) assist the surgeons daily in the operating room. While they do not perform the operations alone in the OR without the surgeon, they work right alongside of the surgeon, and have a knowledge of many of the key steps many basic surgeries entail. They would also be experienced at wound debridement and management, an invaluable skill in a WTSHTF situation.
- Physical Therapists, Physical Therapy Assistants, Radiology Technicians, and Medical Technologists (who run the laboratory) all are usually CPR trained and have knowledge in their respective fields which will have some use to a group.
- Physicians (MD and DO’s), Physician Assistants (PA-C’s), and Nurse Practitioners (NP’s):
- These fields represent the most experienced practitioners. They are the team members who make definitive diagnoses and administer the most complex treatments to patients.
- Work experience and background training can be widely variable, but here are some of the fields (both physicians and PA-C/NP’s) that would be MOST useful to a preparedness group:
- Surgeon (especially Trauma, General, Orthopaedic, ENT, and OB/GYN)
- Emergency Medicine
- Anesthesiologist/Critical Care Intensivist
- Hospitalist
- Cardiologist
- Primary Care (Family Practice, Internal Medicine, Pediatrics)
- Many of these medical professionals have sacrificed a great deal of their free time to train in their specialty, and then work the demanding hours of the job. Due to this, they may not be the best shooter or tactician in your preparedness group. They may not have as deep of knowledge of gardening or mechanical repair work as others. Do not expect them to always be able to contribute in those ways as much as others with more “hands on skills.” What they can do for your group from a medical standpoint will more than make up for these deficits, so long as they are willing to participate in group training/meetings, share in the preparedness planning, and purchase their share of supplies so they aren’t “dead weight” to the group.
- Utilize the group members with medical knowledge to help train the others. It is fairly easy for a medical professional to become CPR or Stop the Bleed “Instructor Certified.” If they could become certified, they could officially instruct the rest of the group.
- Often times these team members also have access to “outdated” medical supplies which would otherwise be thrown out at their jobs. (These supplies are usually perfectly good, but have hit an arbitrary manufacturer expiration date.) Obviously, this acquisition needs to be done legally, but many hospitals and EMS services will allow employees to take home outdated supplies for their own use. It may be a great way to add medical supplies to the group.
Affording It:
I acknowledge that many of these medical supplies above can be budget-strainers, especially if bitten off all at once. Here are some tips that may help some readers, depending on your individual budget and insurance situations:
- Preventative Care: The majority of preventative care at the PCP office is covered by many insurance plans now. I urge you to take advantage of this. (This includes your visit with your PCP, necessary preventative labs, and age-related testing such as colonoscopy and mammography.)
- Prescriptions: Cost may be a budget issue filling a large number of Rx all at one time. Several of the large retailers (Walmart, Meijer, Target, Sam’s Club, and Costco) have Rx discount programs where many of these medications are available for very reduced prices. I suggest shopping around a little if you want to invest the time, in order to save some money. (goodrx.com has a good price comparison tool.)
- HSA: If you have a HSA (health savings account), you can receive tax benefits from non-taxable income if you pay with your HSA account. (You can put up to $7,000 into your HSA in 2019 if you have a qualifying HDHP “high deductible health plan”). This can be spent, for you or your qualifying family members, on:
- Prescription and over-the-counter medications
- Medical treatments not covered by insurance (e.g.- LASIK vision correction)
- Dental and Eye care, glasses and contacts, and orthodontic braces
- Any of the medical supplies mentioned in this article, including an AED
- Health Care Coverage: I realize that everyone’s employment and financial situations are different, and with that comes the availability, or lack thereof, of health insurance. However, running without healthcare coverage of some sort leaves you and your family highly exposed to complete financial devastation. I have seen families acquire six-figure debt loads in one emergency event, and I do not want to see this happen to your family. Here are several options to evaluate for your family’s situation:
- Health Insurance: If you have good employer-sponsored (usually highly subsidized by your employer) health insurance, this is often your best option. It may also be your best choice if you are self-employed, especially because it is tax-deductible in many circumstances.
- HDHP with HSA: If your family is blessed with relatively good health, I encourage you to look into the High Deductible Health Plan (HDHP) with HSA option, and fund the HSA as much as possible. This is a highly tax-advantaged account, so it makes good business sense for many to use it as a way to save money for future healthcare needs (including in-home and nursing home care in the future). It also allows you to use it as a “passthrough” to avoid paying taxes on the money you will be putting into your medical preps…just remember to save your receipts. (https://survivalblog.com/letter-re-getting-first-aid-supplies-tax-free/)
- Christian Medical Sharing plans: If you are not able to have employer-sponsored health insurance, this is a good option for many people. While this is not true “insurance” it functions in a similar fashion to protect your family from catastrophic financial devastation in the event of a large medical bill. I have seen it work out well for many families we know personally.
- Medicare: For those 65 or older, Medicare plus a good supplement plan can be your best option. You have paid in to it for your entire working life (the “Medicare tax”), so you should not feel guilt for collecting on this in your retirement years.
- Medicaid, “Marketplace” and/or State-Specific Plans: While many readers probably share my macro perspective that these plans are steps towards a socialized medicine state that I do not agree with, they are other avenues which exist that you might consider if that is your only viable option to provide healthcare to your family and protect against catastrophic financial risk. If these are your family’s only reasonable way to have health coverage, then I encourage you to consider them, rather than to go without health coverage. You simply cannot afford to be without some type of coverage in the event of a major injury or medical condition.
About the Author:
“Doctor Dan” is a board-certified physician anesthesiologist who practices anesthesiology and critical care medicine in a rural hospital. Due to his previous training in trauma surgery, he also maintains an interest in EMS and disaster preparedness medicine. He serves as a Tactical Medical Director for a SWAT team, and as a medical director/training officer for fire departments and EMS services in his area.
Doctor Dan and his family live on a farm, where they hunt and raise a garden. They believe in trusting God, but also doing their part to be prepared so that they can be a help, not a burden, to others when a time of crisis occurs.










Doctor Dan thanks for stressing the training! One of the courses that I find to be a little more extensive and Prepper related are the wilderness first aid or responder courses. The premise of most first aid courses is that the patient can get to the hospital quickly where as the wilderness courses assume that advanced care will be delayed.
Gauze- lots of gauze. A major wound will use up a lot of gauze pads and rollers. A box a pads can be used up in 2-3 days one one wound on one person. How long does it take to heal? Weeks in some cases.
Thanks 3ADscout. I agree on the gauze. It’s cheap, lightweight, lasts a long time (if kept clean and dry in storage).
AWLS (Advanced Wilderness Life Support) is an organization that has a lot of good courses in outdoor medicine/first aid. Plus, their courses are in some pretty cool destinations for those who already love the outdoors!
https://awls.org
So great to see this information, especially the part about how to get training. CERT Training (Community Emergency Response Team) is another program available in many local areas. It’s a great course which also allows for networking with local emergency personnel.
I have seen the SWAT-T tourniquet highly recommended. It is the only tourniquet that can be used on children (as well as adults) and can be applied with one hand.
Israeli Bandage battle dressings and Celox injectors to stop bleeding also are advised. Celox can be broken down by the body and does not have to be removed from the wound like Quickclot does.
YouTube has lots of videos on how to apply tourniquets and bandages. If you have little to no medical training, you should at least have some idea how to use a tourniquet and Israeli bandage in an emergency until you can get more knowledgeable assistance.
I think training here is a big thing. An AED is only as useful as the person using it. The bigger problem is treating the cause of the cardiac arrest and managing care post arrest care down the line otherwise you could very well just be prolonging the inevitable 🙁
On another note….the poor mans defib…..whats your thought on teaching the precordial thump?
There are many treatable cardiac arrest causes where early defibrillation not only saves lives, but also brain function. If you live in a remote area, there is no way that an ambulance or VFD will be able to arrive fast enough to defibrillate the victim out of the ventricular fibrillation. If you own one and have it easily accessible, it is possible that you might save a life and brain. I would advocate for owning one, as my family personally has invested in one.
If someone is dying in front of your eyes, and a defibrillator is not available, then what harm does it do to try a “hail mary” precordial thump. If it doesn’t work, the patient is no more dead than he would be had you not given it a try!
Thanks for an excellent overview.
One critical area I found when serving overseas as an advisor, is our lack of recognition of basic Preventive Medicine, especially in the US. We take it for granted and fail to plan for grid-down.
I spent two tours, advising Afghan National Police Central Region Commander, and Afghan National Army 201st Corps. Lack of hygiene in urination and defecation, food preparation, and water consumption were causing over 23,000 days of soldiers too sick to report for duty in the 201st Corps. That is in conditions far more sanitary than you will have in TEOWAWKI.
PM is a critical skill for each person, requiring absolute discipline in practice, from the individual survivalist, to anyone touching food, to the person cleaning the surgery and instruments.
Far more of us will die in bed with intense fever and sweats, while painfully violently vomiting, with diarrhea uncleaned, than from trauma. Even if you are careful yourself, one careless contagious person will gift you those wonderful things.
When I was a battery (company grade) commander feeding in the field I personally made each soldier wash his hands if he wouldn’t do it voluntarily at the wash station set up at our feeding location.
My First Sergeant should have done it but he was too chummy with the men.
We had far less cases of diarrhea than other, undisciplined units. When MRE’s are getting used, you have less issue because the men eat from the pouches with an individual spoon they usually throw away. But
You may recall photos of Viet Nam where guys had their spoon sticking out of their pocket so the could reuse it. Spoonfuls of gut torture if you don’t sterilize it before sticking it in your pie hole.
But things aren’t trouble free by using MREs because you cannot ensure that wash feces and urine off their hands before they eat or put tobacco in their mouths. You still get people with violent vomiting and diarrhea that contaminate areas, and thus potentially infecting everyone else who gets exposed.
After my advisor tour with the ANA, I gained a whole new respect for Preventive Medicine. It is a true combat effectiveness multiplier.
The point becomes critical for you at your retreat. If you need three people on watch and one is sick at the latrine for hours, the illness is the same as you being attacked by a machinegun instead of a rifle. You can fight off a rifleman, but you probably can’t fight off a machinegun-like violent illness that will defeat your small force.
God Bless and keep the TP and soapy water handy.
I can’t agree with Dr Dan more regarding pre-screening. Early detection of prostate cancer probably saved my life. While it couldn’t have been caught any earlier, one of the 2 locations it was found was 2mm from the edge. If it had moved outside, all bets would have been off. See you doctor for routine testing and blood work!
Joining local fire department you get all of your training free or low cost. You might have to take additional classes but firefighter / EMR is great tools to have in your tool box. CERT ( COMMUNITY EMERGENCY RESPONSE TEAM) is another tool.
Really good advice Wheatley, I was just re thinking my experience as a medic back in the day. I might not be the best guy in the group for tactical decisions but field sanitation is equally important. Our motto back then was To Preserve the Fighting Strength”.
Colleen you are so right on about post event care. As a former ER RN I’d add that the most important thing to add to the AED would be an oxygen generator. Most of them run off of 12 volts so a way to recharge the battery would also be important. Not cheap but the first medication to give with a heart attack is oxygen and for advanced cardiac life support, oxygen is considered to be a medication.
Doom and Bloom is another website to be familiar with.
Thanks for the excellent insight Doctor Dan
Colleen
I have successfully used a precordial thump many times over 30 years as a critical care nurse, while waiting on a crash cart. I also agree with you about an AED, these are only a stop gap if there is no where to transport for higher level cardiac care, as most arrests are from coronary artery disease. Although I would love to have an AED at home, the expense is too high for the average family/group, and first line cardiac drugs mostly impossible to have on hand……let alone a cath lab at home!! BUT, for times when a cardiac arrest is due to electrocution via lightning strike or electrical accident or hit to the chest such as you sometimes see in baseball accidents, an AED would be a great asset. Undiagnosed cardiac abnormalities seen in young athletes (mostly males) would also fall into this category. Understanding the fact that the 99% of people will probably not have access to an AED in these instances I would not hesitate to try a precordial thump, although it fell out of favor and is not really taught anymore, i’ve seen it work to many times to not try it. I was an ACLS instructor for about 20 years and we did used to teach it. I have not looked but I would not be surprised if there were YouTube videos out there that can demonstrate this relatively easy procedure. The cardiac rhythm seen most often in the above scenarios is usually ventricular fibrillation and using a thump very quickly may just work. I’m not a doctor (but I did stay at a Holiday Inn last night), so take this only as a method to use in a very austere environment.
STEMI and Non-STEMI (types of heart attacks), drowning, lightning strike, electrocution…all of these patients could benefit from early defibrillation with a home AED!
I agree that a precordial thump is better than watching someone surely die (brain death occurs within about 5 minutes of the onset of V-Fib), although neither a precordial thump nor an AED is a guarantee that someone will live. It just increases their chances of living through said events.
If you can get someone back into a normal rhythm from V-Fib in a timely fashion, you can save their brain along with their life.
If I drop over, I hope someone does me the courtesy of early defibrillation!
Me too Doctor Dan! I hope someone can give me early defibrillation also, and I would LOVE to have an AED at home. I also would dearly love that if someone is doing CPR on me that they do CPR & breathing for me, I’m very afraid that if I had some brain damage that I may be able to have respiratory function off of a ventilator, so my husband would not just be able to unplug me!!!
Precordial thump
More info…..if I witnessed let’s say somebody falling over in the grocery store and I actually again “witnessed “ this, I would check their pulse, and if pulseless I would still try this as quickly as possible…the quicker the better. If they had family around them I would also be asking some very quick questions as to their medical history to see if I could rule out other causes for their arrest. Ask for an AED and have someone calling 911 while starting CPR. My next statement is on current recommendations for CPR, they now recommend only doing the chest compressions. My personal opinion on this is if your not going to breathe for me, please do not do chest compressions for me, I do not want to end up as a vegetable, I understand why they recommend this because people are so paranoid about catching something from someone they don’t know if they have to breathe for them. All the crazy things you are thinking you are going to catch, you are not, maybe possibly a cold, or some might say herpes simplex 1 (a cold sore) if you are an adult you have already been exposed to herpes numerous times, you already have a history of this or not but the likelihood of catching it as an adult is probably pretty small. Our lungs have about a 5 min reserve of air, after that time if they are not getting any air you start to have an anoxic brain injury, to what extent it depends on how long your go without oxygen. Remember. …you are trying to save a life, try to save it intact as much as possible! I can honestly say I would not have trouble breathing for a stranger. This is totally my honest opinon.
Just had a brief from our fire chief and EMT today, stating with chest-compression-only CPR, until the ambulance crew takes over, they estimate 80% of patients will live, as opposed to other method incorporating breathing just getting 10% lives saved.
Wheatley
I’m not saying don’t do CPR, but the BEST form of CPR is chest compressions and rescue breathing, especially if you have a second person on the scene. I have many years of experience of seeing CPR delayed or only chest compressions being done, and by the time EMS gets there or when they arrive in the ER and are given correct CPR and first line cardiac drugs, YES they are alive, and are quickly transferred up to ICU on a ventilator, many times cardiac arrest happens again due to the drugs wearing off. Depending on how long their “down” time was (how long before CPR was started or EMS arrived) has everything to do with how much brain can be saved. You would never see EMS personnel, or hospital staff doing only chest compressions. The American heart association changed to chest compressions only for the public because of people’s fear of breathing for a stranger. The majority of people probably live out side of that 5 to even 10 min. distance, I know I sure do. Even in large cities with massive traffic jams, it takes some time to reach a victim. My point in saying “don’t do chest compressions for me if you are not going to breathe for me” is because if I survive, I want to survive with an intact brain! I’ve seen way too many people with anoxic brain injuries. People need to get over their fear of rescue breathing. Everybody needs to take a CPR class every 2 years at least for your family, friends and strangers. What your chief does not see is nurses like me who deal with grieving family members when their loved one is brain dead and we eventually turn that ventilator off.
TXnurse, I concur 110%! Hypoxic means loss of function and i have seen way too many impaired or brain dead people after a “successful” resuscitation.
Sorry, but I’ll take my chances. Defibrillate or precordial thump me…my wife can unplug me from life support a few days later if my brain didn’t make it!
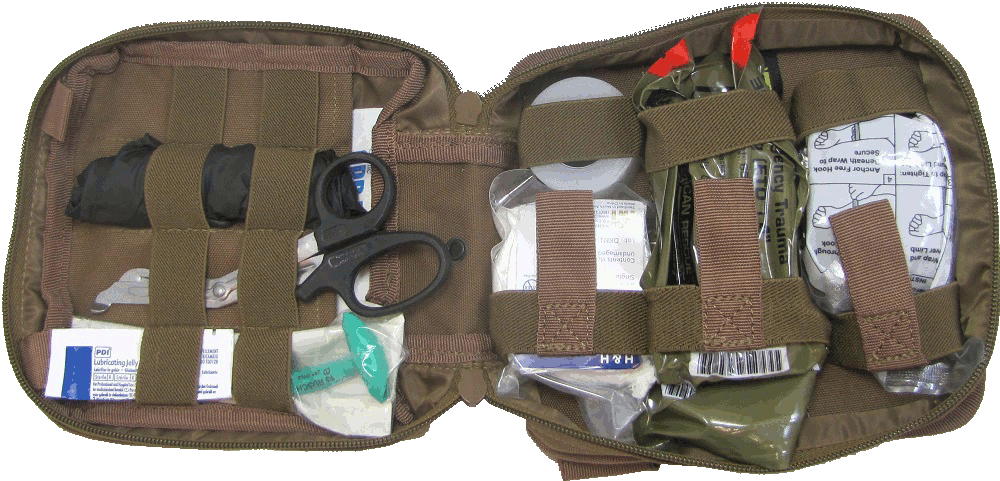
Regarding IFAK contents, here is what I carry in mine (and my wife carries in hers). Feel free to modify your own, it’s just one possibility:
Pouch
Tourniquets x 2
Chest seals x 2
Olaes/Israeli Battle banadages
Quickclot
Angiocaths 14 ga x 2
Scalpel
2-0 silk suture on Keith (straight) needle
Trauma shears
Hemostats
CPR masks
Nasal airway
Oral airway
TCCC cards
Marker
Regular bandages
Nitrile Gloves